The road home

One Saturday in early July, when you were likely asleep, Arianna (McClain) Shirk ’02 was dancing joyously in AIC Kijabi Hospital’s neonatal intensive care unit in Kijabi, Kenya. Calming the labored breathing of a 1-pound infant, struggling to survive hours after birth, tends to have that effect on emergency pediatric physicians.
The child’s life may have been saved by the donation earlier that day of a nasal cannula–a device used to deliver supplemental oxygen–that Shirk had never seen before, one with extra-small plastic tubes that could fit in the baby’s tiny nostrils. Previously, the hospital had nothing like it, and when she realized what was needed Shirk didn’t bark orders at a nurse—she ran home and retrieved the necessary parts from her bedroom floor. Because that’s what doctors do in Kenya.

Arianna examining a tiny patient in AIC Kijabi Hospital’s neonatal intensive care.
Shirk didn’t know that when she pronounced to her parents, at the age of 5, she was going to live in Africa when she grew up. But odds are, if she had it would only have deepened her desire to move to a place where some part of her has always known she was supposed to be.
“That really was what I said,” Shirk recalls, and nothing since has made her waver. Kijabi means “Place of the Wind” in Maasai, and it rises almost 7,000 feet above sea level–higher than any place in North America east of the Mississippi River–on the edge of east Africa’s Great Rift Valley. A 3,700-mile long trench dividing the continent, the Valley is one of the few barriers massive enough to symbolically rival the one between the resources available to doctors in the U.S. and to those in Kenya.
AIC Kijabi Hospital has 363 beds and five of the country’s approximately 100 ICU beds. Knowing that 46 million people live in Kenya provides perspective. Nearly all of its supplies are donated, as is Shirk’s salary.
“A lot of my families live on somewhere between $30 and $40 a month, so every test I order, everything I do, every day they stay in the hospital, means they can’t feed their other children, they can’t pay their rent, they can’t plant their crops,” Shirk says. “Those are the unbelievable sociological and ethical issues that I have to consider every day.”
Fortunately for her patients, Shirk has been considering those issues since her days as an undergraduate, thanks to the unique opportunities Furman presented and she pursued. Shirk “really, really” wanted to attend Furman after a scholarship interview, and once on campus she took advantage of the Individualized Curriculum (ICP) Program to design a major that would allow her to become exactly the kind of doctor she intended to be.
“I knew I wanted to practice medicine in a resource-limited setting, and I think I’m literally the only person that’s ever graduated from Furman with that major,” Shirk says, referring to her bachelor of science in perspectives on poverty and health. “But I circled everything I wanted to take in the catalogue and figured out a way to make it happen.”
One of the classes that got the red-marker treatment was The Medicine Program, a medical ethics and medical sociology course co-taught by sociology professor Kristy Maher, Ph.D., and philosophy professor Carmela Epright, Ph.D. Thought to be the only program of its kind on the country, The Medicine Program puts students in medical facilities trailing doctors and other healthcare professionals as they make difficult real-world decisions. Hands-on, high-impact programs like these are part of Furman’s promise to every student through The Furman Advantage.
“I did design my major around their class … (because) I felt like being able to get that perspective was incredibly important before I started practicing medicine,” Shirk says. “I didn’t understand diabetes. I didn’t understand a urinary tract infection or a heart attack, but I could look at the dynamics of the family, and I could look at how things were affecting the families separate from medicine.”
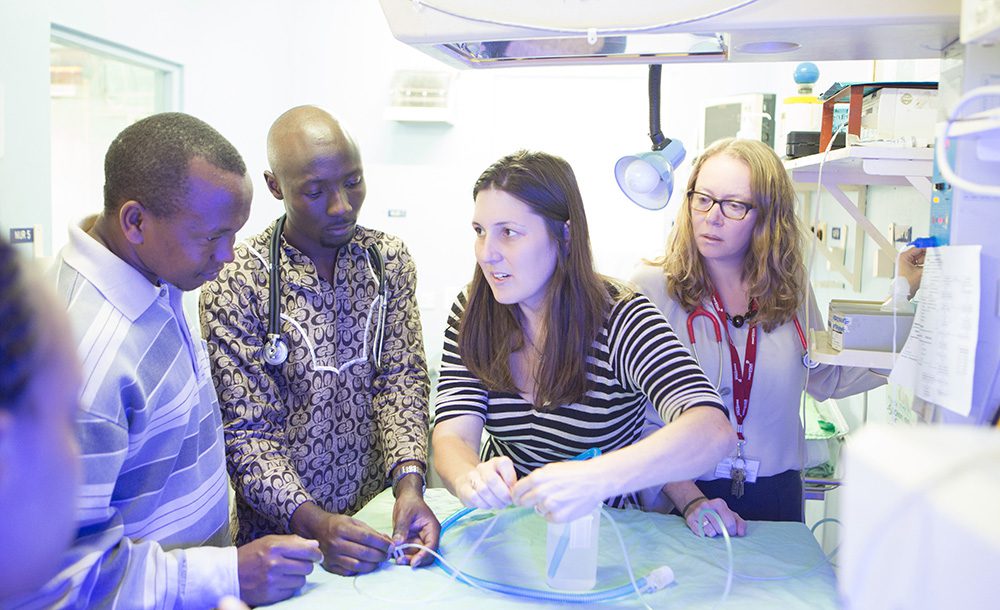
Arianna teaching former interns to build bubble c-pap tubing for use at field hospitals.
Shirk went on to earn a prestigious Harry S. Truman Scholarship and attend the Wake Forest School of Medicine in Winston-Salem, where she grew up, focusing on pediatric emergency medicine. During her residency in Alabama, Shirk briefly wondered if she should devote herself to America’s inner cities, but a year in Taiwan as a Luce Scholar with husband David Shirk ’02, whom she’d married less than a month after both graduated from Furman, refocused her lenses.
In 2013, the couple and their daughters, Madeline and Annabelle, visited Kijabi. Their path was set.
“I called my parents and told them we were planning on moving,” Shirk says. David knew it was coming, and on some level Arianna’s family did too. Still, the realization of her lifelong dream didn’t come without some trepidation.
Shirk signed up for just a two-year commitment to make sure being 8,000 miles away from the life she’d always known was really going to work for the family. They moved in the fall of 2014 as part of Samaritan’s Purse post-residency program, and by the time they returned to America last fall for a mandatory furlough, required to combat burnout, they had their answer.
David, a religion major at Furman, works as a photographer and is the executive director of Friends of Kijabi, the hospital’s non-profit fundraiser. Even more importantly, Madeline (now 11) and Annebelle (8) love their adopted home.
“It’s a daily thing to see monkeys, and we get zebras on the side of the road all the time. It’s like seeing cows,” Shirk says. “I’m still in awe every time we get to go walk with giraffes, but the last time we did it my girls stopped looking at the giraffes to pick flowers. It was like, OK, our life is a little bit different.”
That’s a word Epright uses to describe Shirk. The two have been friends since Arianna was her student, and Epright marvels at her priorities and courage.
“Here’s what she won’t tell you: Emergency pediatric medicine is very rare,” Epright says. “You have to be outstanding to do a fellowship in it, and if she were in the United States she could probably make a half a million dollars a year because there just aren’t pediatric doctors that are trained in emergency medicine … When you’re in Africa, you have nothing, so you have to figure out how to do incredibly complicated medicine … with very limited medication, very limited access. That’s not going into missionary work for a semester. That’s a level of commitment that’s hard to express.”

Arianna and David Shirk ’02 with girls Madeline and Annabelle
Shirk gave a CLP and spoke to Epright’s class when she and David visited campus last fall as part of their whirlwind five months in the United States, which, in addition to a welcome opportunity to attend sister Sandra’s wedding and visit college friends, allowed Madeline and Annebelle to experience North America’s exotic wildlife (“They think squirrels chasing each other is just amazing,” Shirk said with a laugh).
If you think the time in America might also make the Shirks long for home, you’re right. And it was 24 hours of travel away. She signed up for the maximum five-year commitment this time.
“This is where we hope to be for as long as we can see into the future,” Shirk says. “A lot of life is beautifully simple in Kenya, and I get to live on the edge of the Great Rift Valley with these spectacular sunsets every night. A lot of the distraction, a lot of the noise that we deal with in the U.S., is not here. We really feel like this is the call on our lives. This is why I’m a doctor, which is hard to put into words.”
Follow the Shirks by visiting their blog, shirkadventure.com.
Photos courtesy of David Shirk ’02